Introduction: Balance Is Confidence in Motion
Balance is easy to ignore until it starts to feel uncertain.
Maybe you hesitate before stepping off a curb. Maybe stairs feel less automatic than they used to. Maybe you notice yourself reaching for furniture when walking through the house at night. Maybe uneven ground, crowded spaces, quick turns, or carrying groceries suddenly feel more demanding.
That change can be unsettling.
Balance is not just the ability to stand on one foot.
Balance is confidence in motion. It is what allows you to walk, turn, climb stairs, step over obstacles, catch yourself when you stumble, and move through the world without constantly second-guessing your body.
Coordination matters too. Coordination is what helps your arms, legs, eyes, trunk, and nervous system work together smoothly. It is how your body organizes timing, control, rhythm, and accuracy.
The American Heart Association describes balance exercise as one of the four major types of exercise, along with strength, endurance, and flexibility. It also notes that balance is important for everyday activities such as walking and going up and down stairs, and that balance exercises can help prevent falls (American Heart Association [AHA], 2024).
That is why balance and coordination training deserves its own article.
At Royal Blue Fitness, we see balance as a full-body skill. It depends on strength, sensation, vision, inner-ear function, reaction speed, posture, confidence, and repeated practice.
This article will explain what balance and coordination actually mean, why balance changes with age, inactivity, injury, and health conditions, what systems help keep you steady, which exercises improve balance, when balance problems need medical attention, and how Royal Blue Fitness approaches balance and coordination training in Pleasant Hill.
This is general education, not medical advice. If you have dizziness, vertigo, fainting, repeated falls, sudden balance changes, weakness, numbness, vision changes, chest pain, new headaches, or balance issues after injury, speak with a qualified healthcare professional.
What Balance and Coordination Actually Mean
Balance and coordination are related, but they are not the same thing.
Balance is your ability to stay steady.
Coordination is your ability to organize movement smoothly, accurately, and at the right time.
Balance helps you stay upright. Coordination helps you move well.
You use balance when you:
- Stand from a chair
- Walk across a room
- Step off a curb
- Climb stairs
- Stand on uneven ground
- Carry a bag
- Turn around quickly
- Reach overhead
- Catch yourself after a stumble
You use coordination when you:
- Walk with a natural arm swing
- Step around an obstacle
- Catch a ball
- Change direction
- Dance
- Hike over uneven terrain
- Perform a strength exercise with control
- Match breathing with movement
- Move your limbs together without feeling awkward
Good balance is not stillness. It is constant adjustment.
Even when you stand quietly, your body makes tiny corrections. Your feet sense pressure. Your ankles and hips respond. Your eyes scan the environment. Your inner ear tracks head movement. Your muscles and nervous system adjust without you having to think about every detail.
That is why balance is trainable. If the body can learn to coordinate those systems more effectively, steadiness can improve.
Mayo Clinic explains that balance exercises can help people feel more secure, improve stability, and support safer movement at any age. Their guidance also emphasizes using support when needed and progressing balance challenges gradually (Mayo Clinic Staff, 2024).
The key idea is simple:
Balance is a skill. Skills improve with the right kind of practice.
Why Balance Changes With Age, Inactivity, Injury, and Health Conditions
Balance can change for many reasons.
Age plays a role, but it is not the only factor. Inactivity, pain, injury, chronic disease, medication changes, vision changes, inner-ear problems, neuropathy, weakness, joint stiffness, and fear of falling can all affect steadiness.
A person may feel less balanced because:
- Leg strength has declined.
- Ankles and hips feel stiff.
- Vision has changed.
- Foot sensation is reduced.
- Reaction time is slower.
- Walking speed has decreased.
- Medications cause dizziness or lightheadedness.
- An inner-ear condition affects equilibrium.
- A previous fall created fear.
- Pain changed how the body moves.
- A surgery or illness reduced conditioning.
- The person stopped challenging balance regularly.
The National Institute on Deafness and Other Communication Disorders explains that balance disorders can make someone feel unsteady, dizzy, lightheaded, disoriented, or as if they are moving or spinning. It also notes that balance problems may be caused by medications, ear infections, head injury, low blood pressure, skeletal or visual system problems, or issues affecting the inner ear or brain (NIDCD, 2024).
This is why balance problems should not be dismissed as “just getting older.”
Some changes are trainable. Some need medical evaluation. Many require both awareness and a structured movement plan.
Inactivity is one of the biggest hidden contributors.
When someone stops practicing balance, the skill fades. When strength declines, balance becomes harder. When balance feels harder, movement becomes more cautious. When movement becomes more cautious, strength and confidence decline further.
That cycle can quietly shrink a person’s world.
Balance training helps interrupt that cycle by giving the body safe opportunities to practice steadiness, control, and reaction.
The Three Sensory Systems Behind Balance
Balance depends on several systems working together.
The three major sensory systems are:
- Somatosensory system
- Vestibular system
- Visual system
Each one gives your brain information about where you are and how you are moving.
Somatosensory System: Your Body’s Position Sense
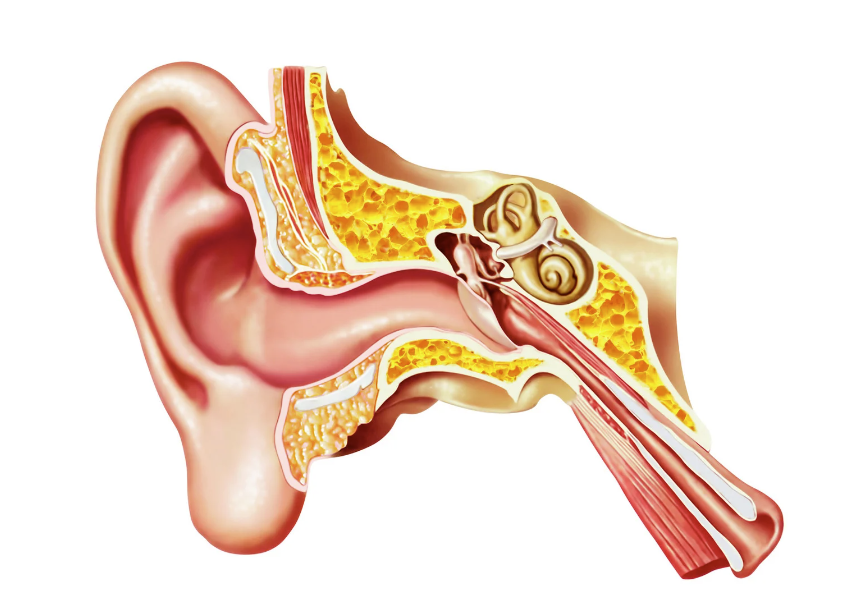
Vestibular System: Your Inner-Ear Balance System
Visual System: Your Eyes as a Balance Tool
Why Strength Matters for Balance
Strength supports balance because different muscle groups help solve different movement problems. Lower-body strength helps you rise from a chair, climb stairs, and recover from a stumble. Hip strength helps control side-to-side movement, especially when stepping, turning, or walking on uneven ground. Ankle strength helps your body make small corrections when the surface changes. Trunk strength helps you stay upright while reaching, carrying, turning, or shifting weight.
The main point is this:
balance is not only a nervous system skill. It is also a strength skill. If the muscles cannot produce enough force, the body has fewer options when it needs to adjust.
Johns Hopkins Medicine explains that exercises focused on balance and strength can reduce fall risk, and it highlights movements such as sit-to-stand, balance holds, and walking-based drills for fall prevention (Johns Hopkins Medicine, n.d.).
Strength matters because balance is not only a nervous system skill. It is also a force-production skill.
If the muscles cannot produce enough force, the body has fewer options.
That said, strength alone is not the entire solution.
A 2021 systematic review and meta-analysis comparing strength training with alternative exercise interventions for fall prevention found no clear difference in falls between strength training and other exercise programs, while noting that the evidence was limited and heterogeneous (Claudino et al., 2021).
The coaching takeaway is important:
Strength training should support balance training, not replace it.
A complete plan combines:
- Lower-body strength
- Hip and trunk control
- Functional stepping
- Balance practice
- Gait confidence
- Coordination
- Reaction training
- Real-world movement tasks
The strongest balance plan is integrated.
Why Coordination and Reaction Time Matter
Balance is not only about holding a position.
Real life moves.
A dog pulls on the leash. A curb appears sooner than expected. A grocery bag shifts weight. Someone bumps into you. Your foot catches the edge of a rug. The ground changes under your feet.
In those moments, the body needs coordination and reaction.
Coordination helps you organize the movement. Reaction time helps you respond before the stumble becomes a fall.
Coordination training may include:
- Stepping patterns
- Arm-and-leg movement drills
- Ball tosses
- Direction changes
- Marching patterns
- Ladder drills
- Controlled agility work
- Carrying while walking
- Turning drills
- Reaching while maintaining stance
Reaction training may include:
- Step-and-catch drills
- Partner cues
- Direction-change cues
- Controlled perturbation exercises
- Obstacle stepping
- Safe “recover your balance” practice near support
Power also matters. Power is the ability to produce force quickly.
A 2022 systematic review and meta-analysis in European Review of Aging and Physical Activity reported that power training was more effective than traditional strength training for improving muscle power in adults 60-plus, while both forms of training may be relevant depending on goals and ability (el Hadouchi et al., 2022).
For everyday life, that matters because catching balance is not always slow. A stumble may require a quick step, a fast weight shift, or a coordinated reaction before the body has time to think through the movement.
This does not mean every person should start with fast drills. Reaction and power work must be scaled carefully. For many people, the starting point is controlled stepping, supported drills, and small challenges that build response capacity without creating unnecessary risk.
The goal is not speed for its own sake. The goal is usable response capacity.
How Balance Problems Show Up in Daily Life
Balance problems do not always show up as obvious falls.
Sometimes they appear as small changes in behavior.
A person may start:
- Avoiding stairs
- Walking slower
- Reaching for walls or furniture
- Feeling nervous in crowds
- Avoiding uneven ground
- Hesitating before curbs
- Feeling unsure while turning
- Avoiding hikes or outdoor walks
- Sitting down to dress
- Avoiding carrying objects while walking
- Taking fewer trips outside
- Feeling anxious in the shower
- Feeling less confident at night
These changes matter because they can lead to activity restriction.
When someone moves less, strength and coordination decline. When strength and coordination decline, balance becomes less reliable. When balance becomes less reliable, fear increases.
The cycle can become self-reinforcing.
Cochrane’s review on exercise for preventing falls in community-dwelling adults found that exercise reduced the rate of falls and the number of people experiencing falls. The review reported that programs reducing falls primarily involved balance and functional exercises, while programs combining multiple exercise types often included balance, functional exercise, and resistance training (Sherrington et al., 2019).
That is why balance should be trained before someone feels desperate.
Balance training is not only for people who fall. It is for people who want to keep moving with confidence.
When Balance Problems Need Medical Attention
Some balance issues are appropriate for fitness training. Others need medical evaluation.
A trainer can help with strength, mobility, coordination, gait confidence, and progressive balance challenges. But dizziness, vertigo, sudden weakness, fainting, neurological symptoms, medication reactions, and unexplained falls need medical attention.
Talk with a healthcare professional if you experience:
- Dizziness or spinning sensations
- Fainting or feeling like you might faint
- Repeated falls
- Sudden balance changes
- New weakness
- Numbness or tingling
- New vision changes
- Severe headaches
- Chest pain
- Shortness of breath
- Confusion or disorientation
- Balance problems after a head injury
- Unsteadiness that worsens quickly
- Balance issues linked to medication changes
NIDCD recommends speaking with a doctor if someone feels unsteady, feels as if the room is spinning, loses balance and falls, feels lightheaded or faint, has blurred vision, or feels disoriented (NIDCD, 2024).
This is especially important because balance problems can come from different systems. Weak hips, vertigo, neuropathy, knee surgery recovery, medication-related lightheadedness, and general deconditioning can all make someone feel unsteady, but they do not call for the same plan.
A good next step depends on the source of the problem. Strength and balance training may be appropriate when the issue is weakness, inactivity, or loss of confidence. Medical evaluation should come first when symptoms involve dizziness, fainting, sudden changes, neurological symptoms, medication concerns, or repeated unexplained falls.
Good balance training starts with knowing when exercise is appropriate and when medical evaluation should come first.
This is paragraph text. Click it or hit the Manage Text button to change the font, color, size, format, and more. To set up site-wide paragraph and title styles, go to Site Theme.
What Balance Training Should Include
Balance training should be progressive, specific, and safe.
A good program should include several layers:
- Static balance
- Dynamic balance
- Strength
- Gait training
- Coordination
- Reaction
- Mobility
- Confidence-building
- Real-life movement practice
Each layer has a purpose.
Static Balance
Static balance is the ability to stay steady in one position.
Examples include:
- Feet together stance
- Semi-tandem stance
- Tandem stance
- Single-leg stance near support
- Standing with head turns
- Standing with eyes focused on a target
Static balance is often the starting point, especially for beginners.
But static balance alone is not enough because daily life is not static.
Dynamic Balance
Dynamic balance is the ability to stay steady while moving.
Examples include:
- Heel-to-toe walking
- Step taps
- Lateral stepping
- Marching
- Step-ups
- Direction changes
- Reaching while standing
- Carrying objects while walking
- Walking over or around obstacles
Dynamic balance is closer to real life because most falls happen during movement.
Functional Balance
Functional balance connects balance training to daily tasks.
Examples include:
- Sit-to-stand
- Picking something up safely
- Carrying groceries
- Turning while walking
- Getting in and out of a car
- Stepping over a threshold
- Walking while looking around
- Moving through tight spaces
This is where balance training becomes practical.
Reactive Balance
Reactive balance is the ability to respond when something unexpected happens.
Examples include:
- Quick stepping
- Safe direction-change drills
- Partner cue drills
- Controlled perturbations
- Obstacle response drills
Reactive balance should be introduced carefully and safely. It is not where everyone starts, but it is an important ability for real life.
Confidence and Fear Reduction
Fear of falling can change movement.
People may stiffen up, shorten their steps, avoid turning, stop walking outdoors, or reduce activity. Balance training should help build confidence gradually by creating successful experiences.
That means choosing progressions that are challenging enough to create adaptation, but safe enough to avoid panic.
A good balance program does not just test balance. It teaches balance.
Regular assessment of balance and coordination is crucial for identifying strengths and weaknesses in these areas and developing effective training programs. Standard methods and tests used to evaluate these skills include:
- Berg Balance Scale: A widely used test in clinical settings that assesses static and dynamic balance abilities through various tasks like standing up from a seated position, standing on one foot, and leaning forward.
- Timed Up and Go (TUG) Test: This test measures the time it takes for an individual to rise from a chair, walk a short distance, turn around, walk back to the chair, and sit down. It helps assess mobility, balance, and fall risk.
- Dynamic Gait Index (DGI): Evaluates an individual's ability to modify balance while walking in the presence of external demands, such as changing walking speed, turning the head, or negotiating obstacles.
These assessments are vital in tailoring exercise programs to individual needs, monitoring progress, and adjusting training regimens to optimize balance and coordination outcomes.
Stability Exercises: From Supported to Dynamic
Stability exercises should be progressed like strength exercises.
You would not load a heavy squat before someone can control a body-weight sit-to-stand. Balance training should follow the same logic.
Start with support. Then reduce support. Then add movement. Then add complexity.
A simple progression might look like this:
- Stand with both hands on a stable surface.
- Stand with one hand on a stable surface.
- Stand with fingertips on support.
- Stand without support nearby.
- Narrow the stance.
- Add head turns.
- Add reaching.
- Add stepping.
- Add carrying.
- Add direction changes.
AHA gives a similar progression for standing on one foot, beginning with two-hand support, then one-hand support, then one-finger support, and eventually no support once the person is steady (AHA, 2024).
Useful stability exercises include:
- Supported single-leg balance
- Tandem stance
- Heel-to-toe walking
- Step taps
- Sit-to-stand
- Lateral stepping
- Marching
- Clock reaches
- Farmer carries
- Suitcase carries
- Step-ups
- Controlled lunges
- Light agility drills
- Tai chi-inspired weight shifts
Balance tools like foam pads, wobble boards, or BOSU balls can be useful, but they are not required. They are also not the starting point for everyone.
Many people need more strength, better stepping, better gait mechanics, and safer progressions before unstable surfaces make sense.
Mayo Clinic notes that balance exercises can be practiced at home or anywhere, but also emphasizes using a stable object for support when needed and increasing challenge as balance improves (Mayo Clinic Staff, 2024).
That is the safest mindset.
Make the exercise challenging enough to matter, but controlled enough to succeed.
Strength, Gait, and Fall Prevention
Fall prevention is not one exercise.
It is a system.
A strong fall-prevention plan often includes:
- Leg strength
- Hip strength
- Ankle control
- Trunk stability
- Gait practice
- Balance work
- Reaction training
- Vision and environment awareness
- Home safety
- Medication review when appropriate
- Footwear considerations
- Confidence-building
Mayo Clinic’s fall prevention guidance recommends physical activity, medication review, vision checks, sensible shoes, removing home hazards, lighting living spaces, and using assistive devices when needed (Mayo Clinic Staff, 2024).
That broader view matters because many falls have more than one cause.
A person may fall because of poor balance, but the situation may also include dim lighting, loose rugs, rushed movement, medications, weak legs, and poor footwear.
Training can address some of these factors. Environment and medical review may address others.
Exercise still plays a major role.
Healthy People 2030 summarizes evidence from Cochrane showing that exercise programs involving balance, gait, coordination, functional tasks, and muscle strengthening can reduce falls among community-dwelling adults (Office of Disease Prevention and Health Promotion, n.d.).
This supports the same practical point we keep returning to:
The most useful balance training looks like life.
It includes standing, stepping, turning, carrying, reaching, reacting, and recovering.
How Royal Blue Fitness Trains Balance and Coordination in Pleasant Hill
At Royal Blue Fitness, we approach balance and coordination as part of a larger movement system.
We do not treat balance training as a few random drills at the end of a workout. We look at how the person moves, what they are worried about, what they want to keep doing, and which physical qualities need the most support.
Our role is not to diagnose dizziness, vestibular disorders, neurological conditions, or medical causes of falls. Those concerns belong with qualified healthcare providers.
Our role is to help clients build
strength, stability, coordination, movement confidence, and practical balance skills through structured fitness training.
For many clients, that starts with a Strength and Range of Motion Assessment.
That helps us understand:
- Lower-body strength
- Hip and trunk control
- Ankle mobility
- Walking confidence
- Single-leg stability
- Ability to step and change direction
- Posture and alignment
- Strength asymmetries
- Movement hesitation
- Fall history or fear of falling
- Current training level
- Daily-life goals
From there, balance and coordination training may include:
- Supported balance progressions
- Lower-body strength training
- Core and trunk control
- Gait and stepping drills
- Carries
- Dynamic balance exercises
- Reaction and coordination drills
- Low-impact conditioning
- Mobility work
- Confidence-building progressions
The goal is to make balance training useful, not theatrical.
For some people, the most important starting point is learning to stand from a chair with control. Others may need better hip strength, safer stair confidence, gait work, or balance practice near support. More advanced clients may work on directional changes, carrying, low-impact agility, or sport-specific coordination.
The progression depends on the person.
Balance training should help real life feel safer, steadier, and more open.
If you are in Pleasant Hill or nearby in the East Bay and feel less steady than you want to, Royal Blue Fitness can help you build a structured path forward.
FAQ: Balance and Coordination Training
What is balance training?
Balance training is exercise that improves your ability to stay steady, control your body position, and respond to changes in your environment. It can include standing drills, stepping, strength training, gait work, coordination drills, and functional movement.
What is the difference between balance and coordination?
Balance is your ability to stay steady. Coordination is your ability to organize movement smoothly and accurately. Balance keeps you upright. Coordination helps you move well.
Why does balance get worse with age?
Balance can change because of reduced strength, slower reaction time, vision changes, vestibular issues, joint stiffness, medication effects, nerve changes, inactivity, and fear of falling. Age can contribute, but it is not the only factor.
Can balance improve with exercise?
Yes. Balance is trainable. Exercise programs that include balance and functional training have been shown to reduce falls in community-dwelling adults (Sherrington et al., 2019).
What are the best balance exercises?
The best balance exercises depend on the person. Common options include supported single-leg balance, tandem stance, heel-to-toe walking, step taps, sit-to-stand, lateral stepping, carries, and dynamic stepping drills.
Are stability exercises good for fall prevention?
Stability exercises can help, especially when combined with strength, gait, coordination, and functional movement. The most effective fall-prevention programs often include balance and functional exercises.
Is strength training important for balance?
Yes. Strength training supports balance by improving the muscles that help you stand, step, carry, climb stairs, and recover from stumbles. It should be paired with balance and functional movement training.
How often should I train balance?
Balance can be trained several times per week, and simple drills can often be practiced briefly on many days. The right frequency depends on your ability, fall risk, goals, and whether you need supervision.
What causes poor coordination?
Poor coordination can come from inactivity, injury, weakness, neurological conditions, vestibular problems, vision changes, medication effects, pain, fatigue, or lack of practice. Sudden coordination changes should be evaluated medically.
When should balance problems be checked by a doctor?
Balance problems should be checked if they are sudden, worsening, linked with dizziness or vertigo, associated with falls, paired with weakness or numbness, connected to fainting, or happening after a head injury.
How does Royal Blue Fitness train balance and coordination?
Royal Blue Fitness trains balance and coordination through strength training, supported balance progressions, gait and stepping drills, core control, carries, dynamic balance work, mobility, and progressive challenge based on the client’s starting point.
Conclusion: Balance Is a Trainable Form of Freedom
Balance is not just standing still without falling.
It is the ability to move through life with steadiness, awareness, reaction, coordination, and confidence.
It helps you climb stairs, walk outside, carry groceries, travel, exercise, garden, hike, play, work, and stay active without feeling like every step requires negotiation.
Balance can change over time, but it can also improve with the right plan.
A strong balance and coordination program should include:
- Strength
- Static balance
- Dynamic balance
- Coordination
- Gait and stepping practice
- Reaction training
- Mobility
- Functional movement
- Confidence-building progression
The goal is not to perform circus tricks or stand on unstable surfaces just because they look difficult. The goal is to build a body that can handle real-life movement with more control.
At Royal Blue Fitness, we help clients train balance as part of a complete strength and movement system. If you want to feel steadier, move better, and trust your body more, balance and coordination training can be a powerful place to begin.
Power in Progress, Meaning in Motion.
Resources for Fall Prevention and Balance
To further explore balance, coordination, fall prevention, and stability training, here are some reliable resources:
- General Balance and Fall Prevention Information:
- Mayo Clinic Balance Exercises: Explains how balance exercises support stability, independence, and fall prevention.
- American Heart Association Balance Exercise: Describes balance exercise as one of the four major exercise types and gives simple balance practice examples.
- Johns Hopkins Medicine Fall Prevention Exercises: Provides practical strength and balance exercises for reducing fall risk.
- Mayo Clinic Fall Prevention: Reviews physical activity, home safety, footwear, medication review, and vision checks for fall prevention.
- Balance Disorders and Vestibular Information:
- NIDCD Balance Disorders: Explains balance disorder symptoms, causes, diagnosis, treatment, and when to seek medical help.
- Cleveland Clinic Vestibular System: Explains how the inner-ear vestibular system helps maintain balance and coordinate movement.
- Research on Balance Training and Fall Prevention:
- Cochrane Exercise for Preventing Falls: Reviews evidence showing exercise can reduce falls among community-dwelling adults.
- Healthy People 2030 Evidence-Based Resource on Exercise and Falls: Summarizes evidence for balance, gait, functional task, and muscle-strengthening exercises in fall prevention.
- Strength Training to Prevent Falls Systematic Review: Reviews evidence comparing strength training with other exercise programs for fall prevention.
- Power Training Compared With Strength Training Systematic Review: Reviews power training and strength training outcomes in adults 60-plus.
- Physical Activity Interventions for Strength, Balance, and Falls in Middle-Aged Adults: Reviews research on strength, balance, and fall-related outcomes in middle-aged adults.