Navigating Sciatica: Strategies for a Pain-Free Life
Introduction: Sciatica Is More Than Back Pain
Sciatica can change the way you move through your day.
It can make sitting uncomfortable, driving stressful, walking uncertain, and simple movements feel risky. For some people, it starts as a dull ache in the low back or hip. For others, it feels sharp, electric, burning, or like pain is shooting down the back of the leg.
That uncertainty is part of what makes sciatica so frustrating.
You may wonder:
- Is this a back problem, a hip problem, or a nerve problem?
- Should I stretch it or leave it alone?
- Is walking good or bad?
- Can I strength train with sciatica?
- When is sciatic nerve pain serious enough to see a doctor?
Sciatica is not ordinary muscle soreness. It is a pattern of nerve-related symptoms that often starts in the low back or buttock and can travel down the leg. MedlinePlus describes sciatica as a symptom of a problem with the sciatic nerve, with pain, weakness, numbness, or tingling that can start in the lower back and extend down the leg, calf, foot, or toes, usually on one side of the body. (MedlinePlus, 2024)
That does not mean every case is dangerous. Many cases improve with time, medical guidance when needed, movement, exercise, and better load management. But the right approach depends on the cause, the severity, the symptoms, and how your body responds.
The goal is not to guess harder. The goal is to understand what sciatica is, respect the nerve, keep the body moving safely, and rebuild strength with a plan.
This article will explain what sciatica means, what it feels like, what causes sciatic nerve pain, when it needs medical attention, how diagnosis works, how exercise can help, and how Royal Blue Fitness supports back pain management in Pleasant Hill.
This is general education, not medical advice. If you have severe or worsening symptoms, weakness, numbness in the groin or rectal area, bowel or bladder changes, fever, unexplained weight loss, recent trauma, or pain that is not improving, seek medical care promptly.
What Sciatica Actually Means
Sciatica is not a single diagnosis.
It is a symptom pattern.
The American Academy of Orthopaedic Surgeons explains that sciatica is a broad term for nerve pain, not a specific diagnosis. The diagnosis is usually the cause of the nerve compression, such as a herniated disk or spinal stenosis (American Academy of Orthopaedic Surgeons [AAOS], n.d.).
That distinction matters.
When someone says, “I have sciatica,” they are usually describing pain, tingling, numbness, burning, or weakness that travels along the path of the sciatic nerve. But the reason for that irritation can vary.
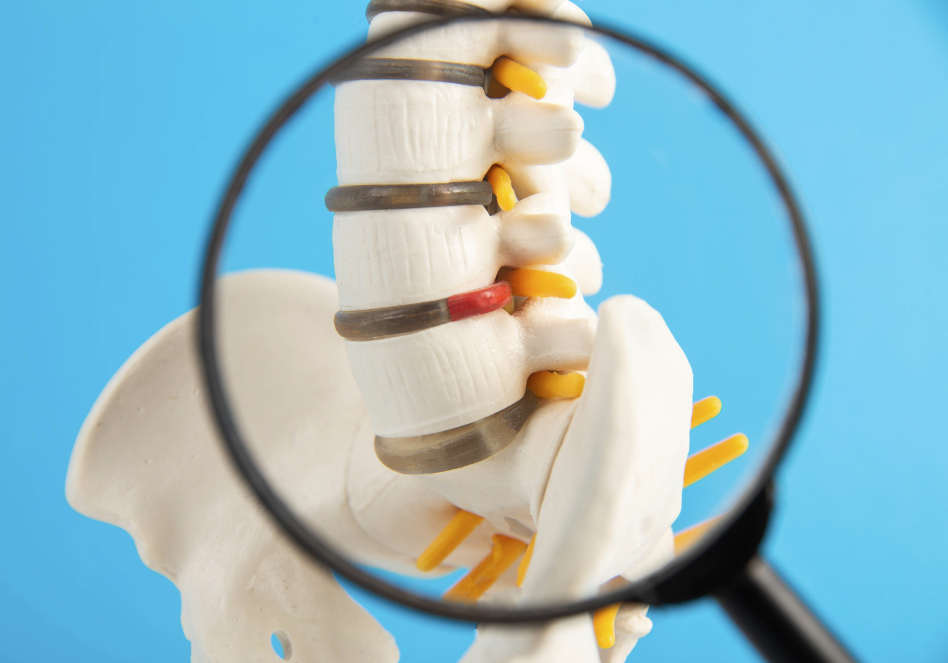
The sciatic nerve is the largest nerve in the body. It forms from nerve roots in the lower spine, then travels through the buttock and down the back of the leg. It helps control muscles in the back of the knee and lower leg and provides sensation to parts of the thigh, lower leg, foot, and toes (MedlinePlus, 2024).
That is why sciatica can feel like more than back pain.
The symptoms may travel.
They may change with position.
They may feel nerve-like instead of muscle-like.
A person with sciatica may feel symptoms in the:
- Low back
- Buttock
- Hip area
- Back of the thigh
- Calf
- Foot
- Toes
The pain can be mild and annoying, or severe enough to interfere with walking, sitting, sleeping, and working.
Sciatica tells you a nerve is irritated. It does not automatically tell you why.
That is why good sciatica management starts with clarity.
What Sciatica Feels Like
Sciatica can feel different from person to person.
Some people describe it as:
- Sharp
- Burning
- Electric
- Shooting
- A deep ache
- Pins and needles
- Numbness
- Weakness
- A cramp-like pain down the leg
Harvard Health describes sciatica as pain that begins in the low back and spreads through the buttock, leg, calf, and sometimes the foot. It can feel dull, aching, burning, tingling, numb, or weak in the affected leg (Harvard Health Publishing, 2024).
Common patterns include:
- Pain that travels down one leg
- Symptoms that worsen with sitting
- Symptoms that worsen with coughing or sneezing
- Pain that improves with walking or changing position
- Tingling or numbness in the leg or foot
- Weakness when lifting the foot, pushing off, or climbing stairs
- A feeling that the leg is not fully trustworthy
Some people feel low back pain and leg pain together. Others mainly feel leg pain. Some people have more numbness than pain. Others feel pain but no obvious weakness.
This variety is one reason sciatica can be confusing.
It is also why a one-size-fits-all exercise list can backfire.
The right plan depends on what your symptoms do, what positions aggravate them, and what movements help them calm down.
Common Causes of Sciatic Nerve Pain
Sciatic nerve pain usually happens when a nerve root in the lower spine is irritated or compressed.
Common causes include:
- Herniated disk
- Spinal stenosis
- Bone spurs
- Degenerative changes in the spine
- Spondylolisthesis
- Trauma or injury
- Pregnancy-related pressure or changes
- Piriformis-related irritation in some cases
- Inflammation around the nerve root
AAOS notes that people under 40 often experience sciatica due to a herniated disk, while adults later in life more commonly experience sciatica related to bone spurs and arthritis (AAOS, n.d.).
A herniated disk is one of the more common causes. The disks in the spine act like cushions between vertebrae. If a disk bulges or herniates, it may irritate or press on a nerve root. When that irritated nerve root contributes to the sciatic nerve, pain can travel down the leg.
Spinal stenosis is another common cause, especially as people age. It involves narrowing of the spinal canal or nerve pathways, which can put pressure on nerves.
The key point is this:
Sciatica is not always caused by the same structure.
That means treatment can differ. Some people need medical care first. Some need physical therapy. Some need time and gradual movement. Some need strength training after the acute irritation settles. Some need help changing how they sit, bend, walk, lift, or train.
The mistake is assuming that every case of sciatica needs the same stretch, the same exercise, or the same timeline.
When Sciatica Needs Medical Attention
Many cases of sciatica improve with conservative care, but some symptoms require urgent medical evaluation.
Call a healthcare professional promptly if symptoms are worsening, interfering significantly with daily life, or not improving.
Seek urgent care immediately if you experience:
- Sudden or severe weakness in one leg
- Numbness in the groin, saddle area, or rectal area
- Loss of bladder or bowel control
- Fever with back or leg pain
- Recent major trauma
- Unexplained weight loss
- History of cancer with new back or leg symptoms
- Progressive numbness or weakness
- Severe pain that is rapidly worsening
Harvard Health recommends calling a doctor immediately for sudden extreme leg weakness, numbness in the groin or rectum, or difficulty controlling bladder or bowel function, because those symptoms may indicate compression of nerves leading to the pelvis and can cause permanent damage if not treated promptly (Harvard Health Publishing, 2024).
This section matters because sciatica content can sometimes become too casual.
Not all nerve symptoms should be stretched, trained through, or “waited out.”
Red flags need medical care.
For non-emergency cases, a healthcare professional can help determine whether imaging, medication, physical therapy, injections, or other care is appropriate.
How Sciatica Is Diagnosed
Sciatica is usually diagnosed through a combination of symptom history and physical examination.
A healthcare professional may ask:
- Where does the pain start?
- How far down the leg does it travel?
- Does it feel sharp, burning, electric, numb, or weak?
- What makes it worse?
- What makes it better?
- Did it begin after lifting, twisting, sitting, injury, or illness?
- Do you have weakness, numbness, bowel or bladder changes, fever, or other red flags?
A physical exam may include checking:
- Muscle strength
- Reflexes
- Sensation
- Walking pattern
- Heel walking
- Toe walking
- Squatting and rising
- Straight-leg raise or other nerve tension tests
Mayo Clinic explains that during an exam, a healthcare professional might check muscle strength and reflexes, including asking the person to walk on toes or heels, rise from a squat, or lift one leg at a time while lying down. Imaging such as X-ray, MRI, CT, or EMG may be used when pain is severe or not improving within a few weeks (Mayo Clinic Staff, 2024).
That last point is important. Not every person with sciatica needs immediate imaging.
The NICE guideline for low back pain and sciatica recommends not routinely offering imaging in a non-specialist setting and explains that imaging in specialist settings should be considered only if the result is likely to change management (National Institute for Health and Care Excellence [NICE], 2020).
That can surprise people.
Many assume an MRI is always the first step. But imaging findings do not always match symptoms perfectly. Some people have disc changes with no pain. Others have significant symptoms with subtle findings. Medical context matters.
The goal of diagnosis is not just to see something on a scan. The goal is to understand what is causing the symptoms and what should be done next.
Why Movement Matters, But Random Exercise Can Backfire
When sciatica hurts, the natural instinct is to avoid movement.
That is understandable. Pain makes the body protective.
But too much rest can create its own problems: stiffness, fear, weakness, deconditioning, and reduced confidence.
AAOS advises that it is important to continue moving, avoid staying in bed too long, find comfortable positions, and be as active as possible because motion helps reduce inflammation (AAOS, n.d.). NICE also recommends tailored advice and information to help people self-manage low back pain with or without sciatica, including encouragement to continue normal activities (NICE, 2020).
But that does not mean all movement is helpful.
Random exercise can backfire if it increases nerve irritation.
For example, some people flare up with:
- Aggressive hamstring stretching
- Deep forward bending
- Heavy deadlifts too early
- Long sitting after exercise
- High-impact cardio during a flare
- Twisting under load
- Stretching into sharp nerve pain
- Exercises that push symptoms farther down the leg
A useful rule is:
Exercise should help symptoms centralize or calm down, not push symptoms farther down the leg.
Centralization means symptoms move out of the leg and closer to the back or become less intense. That is often a better sign than chasing a stretch sensation.
Peripheralization means symptoms travel farther down the leg or become more intense. That is usually a warning sign to stop and reassess.
The right movement plan should respect irritability.
During a high-irritability phase, the goal may be simple:
- Calm symptoms
- Keep walking tolerable
- Avoid positions that flare the nerve
- Maintain gentle mobility
- Reduce fear
- Build a safe baseline
Later, the goal changes:
- Restore strength
- Improve trunk control
- Rebuild hip capacity
- Improve movement tolerance
- Return to lifting, training, work, and recreation
Sciatica exercise is not about finding one magic stretch. It is about matching the movement to the phase you are in.

Sciatica Pain Relief Exercises: What They Should Accomplish
Sciatica pain relief exercises should have a purpose.
They are not just random stretches. They should help the body do one or more of the following:
- Reduce nerve irritation
- Improve comfortable movement
- Restore confidence
- Support the spine and hips
- Build tolerance to walking, sitting, bending, and lifting
- Reduce fear of movement
- Prepare the body for progressive strength training
The NICE guideline says exercise programs for low back pain with or without sciatica may include biomechanical, aerobic, mind-body, or combined approaches, and should account for a person’s needs, preferences, and capabilities (NICE, 2020).
That gives us an important coaching principle:
The best sciatica exercise is not the one that looks best online. It is the one your body tolerates and can progress from.
Common exercise categories include:
Gentle Positioning and Mobility
This may include positions that reduce symptoms, gentle spine motion, or hip movement that does not increase leg pain.
Examples may include:
- Supported walking
- Gentle prone or side-lying positions
- Pelvic tilts
- Cat-cow variations
- Gentle hip mobility
- Short movement breaks from sitting
Nerve Mobility, When Appropriate
Some people benefit from carefully dosed nerve glides or neural mobilization.
A 2023 systematic review and meta-analysis found that neural mobilization was associated with reduced pain intensity and improved disability in people with lumbar radiculopathy, but this kind of work should be dosed carefully because nerves can be sensitive (Hussain et al., 2023).
The practical version:
Nerve mobility should feel gentle, not aggressive.
You are not trying to yank on the nerve. You are trying to restore tolerance.
Core Control
Core work for sciatica is not about doing endless crunches.
It is about improving the way the trunk supports the spine during movement.
Examples may include:
- Dead bug variations
- Bird dogs
- Side planks
- Pallof presses
- Carries
- Breathing and bracing drills
Hip Strength
The hips are important because they help share load with the spine.
Examples may include:
- Glute bridges
- Hip hinges
- Step-ups
- Supported split squats
- Cable pull-throughs
- Hip abduction work
- Squat variations
Low-Impact Conditioning
Low-impact aerobic work can help maintain fitness without adding excessive stress.
Examples include:
- Walking
- Swimming
- Cycling if tolerated
- Elliptical
- Water exercise
Sciatica exercise should be guided by symptoms, not ego.
If an exercise makes symptoms sharper, farther down the leg, or more intense afterward, it may not be the right choice right now.
Strength Training, Core Control, and Hip Support
Strength training can be a powerful part of long-term sciatica management, but the timing and exercise selection matter.
During an acute flare, heavy lifting may not be appropriate. The nerve may be too irritated, and the body may guard against movement.
But after symptoms calm, rebuilding strength becomes essential.
Why?
Because weakness and poor movement tolerance can make the back and hips more vulnerable to future flare-ups.
Strength training can help improve:
- Hip support
- Trunk control
- Glute strength
- Back endurance
- Leg strength
- Lifting mechanics
- Confidence with movement
- Load tolerance
Cochrane’s review of exercise for chronic low back pain concluded that exercise treatment is probably more effective than no treatment, usual care, or placebo for pain, and may improve function compared with no treatment or usual care (Cochrane, 2021).
That does not mean exercise is a cure-all for every case of sciatica. Sciatica can be more specific than general low back pain, especially when nerve compression or radiculopathy is present. But it does support the broader principle that exercise is often part of the solution for persistent back-related problems.
A back-friendly strength plan may include:
- Squat pattern
- Hip hinge pattern
- Step-up pattern
- Rowing pattern
- Pressing pattern
- Carrying pattern
- Core control
- Balance and coordination
The first goal is not maximum load.
The first goal is control without symptom escalation.
A good progression might move from:
- Supported positions to less supported positions
- Body weight to light external load
- Short range to fuller range
- Slow tempo to more natural speed
- Low volume to more work capacity
- Basic patterns to more real-life tasks
For example:
- A person who cannot hinge without symptoms may start with a hip hinge to a wall or a short-range elevated deadlift.
- A person who cannot squat comfortably may start with sit-to-stand from a higher box.
- A person who feels unstable may start with supported step-ups or carries.
- A person with poor trunk control may start with dead bug variations, Pallof presses, and controlled breathing.
Strength training after sciatica is not about proving toughness. It is about rebuilding trust and capacity.
Walking, Low-Impact Cardio, and Daily Movement
Walking is often one of the most useful tools for sciatica, especially when it is tolerable.
It promotes circulation, reduces stiffness, maintains general fitness, and helps the body avoid the negative effects of prolonged rest.
Harvard Health lists walking and swimming as measures that can help strengthen the lower back and notes that prolonged bedrest can make sciatica worse (Harvard Health Publishing, 2024). AAOS also advises short walks as part of staying active during sciatica recovery (AAOS, n.d.).
But walking should still be scaled.
For some people, a 30-minute walk feels great.
For others, 30 minutes creates a flare.
A better approach is to find the minimum useful dose.
That might be:
- 5 minutes, several times per day
- 10 minutes after meals
- Short walks between sitting blocks
- Walking on flat ground before hills
- Walking with rest breaks
- Walking until symptoms begin to increase, then stopping before the flare builds
Low-impact cardio can also help, depending on tolerance.
Options include:
- Swimming
- Water walking
- Elliptical
- Recumbent cycling
- Upright cycling, if sitting does not flare symptoms
- Easy treadmill walking
The body often does better with frequent, tolerable movement than with long, heroic sessions that create a setback.
This matters for people who sit at work, drive long distances, or spend hours in one position.
Sciatica often dislikes stillness.
Movement breaks may help:
- Stand every 20 to 30 minutes
- Walk briefly before symptoms build
- Use a supportive chair setup
- Alternate sitting and standing if possible
- Avoid long drives without breaks
- Change positions before pain spikes
The goal is not to obsess over posture. The goal is to reduce long periods of nerve-irritating positions.
Lifestyle Factors That Can Help Reduce Flare-Ups
Sciatica management is not only about exercises.
Daily habits matter because they shape how often the nerve gets irritated and how well the body recovers.
Helpful lifestyle factors include:
Sitting Strategy
Sitting often aggravates sciatica because it can increase pressure through the low back and hips.
Try:
- Taking frequent standing breaks
- Using lumbar support if helpful
- Keeping feet supported
- Avoiding deep slouching for long periods
- Avoiding sitting on a wallet or uneven surface
- Adjusting car seat position
- Breaking up long drives
Lifting Mechanics
Lifting is not bad by itself. Poorly matched lifting is the problem.
A better approach:
- Keep the object close
- Use hips and legs
- Avoid twisting under load
- Exhale through effort
- Start with lighter loads
- Build tolerance gradually
Sleep Position
Sleep can influence symptoms.
Some people feel better side-lying with a pillow between the knees. Others prefer lying on the back with support under the knees. There is no universal perfect position. The best position is the one that helps symptoms calm down and lets you sleep.
Weight and General Health
For some people, weight management can reduce load on the spine and improve movement tolerance. This should be framed without shame.
The goal is not punishment. The goal is to reduce strain and improve the body’s ability to move.
Stress and Fear
Pain can make the nervous system more protective.
When someone fears movement, they often move less. When they move less, they lose strength and confidence. When confidence drops, the pain feels even more limiting.
NICE recognizes that persistent low back pain or sciatica can involve psychosocial obstacles to recovery and recommends combined physical and psychological programs in some cases when those obstacles are significant or prior treatments have not helped (NICE, 2020).
That does not mean pain is “in your head.”
It means recovery is physical and emotional.
A good plan should help you feel safer moving again.

How Royal Blue Fitness Supports Back Pain Management in Pleasant Hill
At Royal Blue Fitness, we help people rebuild strength, movement tolerance, and confidence after back pain, sciatica, or post-rehab setbacks.
We do not diagnose sciatica. We do not replace your physician, physical therapist, chiropractor, surgeon, or medical team. If you have red flags, severe symptoms, worsening weakness, or unclear medical issues, you need medical evaluation.
Our role is to help you train safely and progressively within your current capacity.
For sciatica and back pain management in Pleasant Hill, that often means starting with a Strength and Range of Motion Assessment so we can understand:
- What movements feel limited
- What positions aggravate symptoms
- What strength gaps may be present
- How your hips, trunk, and legs are contributing
- How your balance and control look
- What exercises you currently tolerate
- What your daily life demands from your body
- What your medical or rehab team has already recommended
From there, a back-friendly training plan may include:
- Low-impact conditioning
- Core control
- Hip strengthening
- Glute strengthening
- Progressive strength training
- Mobility work
- Breathing and bracing practice
- Lifting mechanics
- Walking and movement consistency
- Gradual return to meaningful activities
We are especially interested in helping clients move from fear and frustration into structure.
Because for many people, the hardest part of sciatica is not only the pain. It is not knowing what is safe.
A thoughtful plan gives you a path.
Not a guarantee. Not a magic fix. A path.
The goal is to reduce irritation, rebuild capacity, and help you trust your body again.
FAQ: Sciatica Pain Relief and Back Pain Management
What is sciatica?
Sciatica is nerve-related pain that travels along the path of the sciatic nerve. It often starts in the low back or buttock and can travel down the back of the leg, sometimes into the calf, foot, or toes.
Is sciatica the same as low back pain?
No. Sciatica can include low back pain, but it usually involves nerve symptoms traveling into the leg. Low back pain may stay in the back, while sciatica often follows a nerve-related pattern.
What does sciatica feel like?
Sciatica may feel sharp, burning, electric, shooting, aching, numb, tingling, or weak. It often affects one side of the body.
What causes sciatica?
Common causes include herniated disk, spinal stenosis, bone spurs, degenerative spine changes, and irritation or compression of nerve roots in the lower spine. The cause matters because it influences the right treatment plan.
Should I rest or keep moving with sciatica?
Most people should avoid prolonged bedrest and continue gentle movement as tolerated. However, severe symptoms, worsening weakness, or red flags require medical attention. The right amount of movement depends on symptom irritability.
Is walking good for sciatica?
Walking can be helpful if it does not worsen symptoms. Start with short, tolerable walks and build gradually. Stop or adjust if symptoms become sharper, travel farther down the leg, or flare significantly afterward.
What exercises help sciatica?
Helpful exercises vary by person, but may include gentle mobility, nerve glides when appropriate, core control, hip strengthening, glute strengthening, walking, and progressive strength training. The best exercise is the one that reduces symptoms or builds capacity without increasing nerve irritation.
What exercises should I avoid with sciatica?
Avoid exercises that increase sharp nerve pain, push symptoms farther down the leg, or create a major flare afterward. During a sensitive phase, aggressive hamstring stretching, heavy bending, twisting under load, or high-impact training may be too much.
Can strength training help sciatica?
Strength training can help when it is introduced at the right time and scaled properly. It can improve trunk control, hip strength, movement confidence, and load tolerance. During acute flares, strength work may need to be modified or delayed.
When should I see a doctor for sciatica?
See a doctor if symptoms are severe, worsening, not improving, or interfering with daily life. Seek urgent care for sudden leg weakness, groin or saddle numbness, difficulty controlling bowel or bladder function, fever, major trauma, or unexplained weight loss.
How long does sciatica take to heal?
Recovery varies. Some cases improve within weeks, especially when related to a herniated disk and managed conservatively. Others take longer depending on the cause, nerve irritation, severity, health history, and whether weakness or spinal stenosis is involved.
Can Royal Blue Fitness help with sciatica?
Royal Blue Fitness can help with back pain management, movement confidence, strength training, hip and core support, mobility, and progressive return to activity. We do not diagnose sciatica or replace medical care, but we can help build a safer training plan around your needs and medical guidance.
Conclusion: Sciatica Recovery Requires the Right Kind of Movement
Sciatica is frustrating because it affects more than the back.
It can affect sitting, walking, driving, sleeping, lifting, training, working, and confidence.
But sciatica does not have to mean you stop moving forever.
The better approach is to understand what is happening, respect the nerve, watch for red flags, keep movement tolerable, and rebuild strength gradually.
The goal is not to force your way through pain.
The goal is to build a system that helps your back, hips, legs, and nervous system tolerate life again.
That system may include medical care, physical therapy, walking, strength training, mobility, better sitting habits, better lifting mechanics, and gradual return to the activities you care about.
At Royal Blue Fitness, we help clients move from uncertainty to structure. If you are in Pleasant Hill or nearby in the East Bay and want help rebuilding after sciatica or recurring back pain, we can help you create a safer, stronger path forward.
Power in Progress, Meaning in Motion.
Resources for Further Reading
For those seeking more information on sciatica, its causes, and management strategies, the following resources offer valuable insights:
- General Sciatica Information:
- American Academy of Orthopaedic Surgeons: Provides detailed information on sciatica symptoms, diagnosis, common causes, nonsurgical treatment, and rehabilitation.
- Johns Hopkins Medicine: Offers a clear overview of sciatica, including causes, symptoms, diagnosis, and treatment options.
- MedlinePlus: Provides patient-friendly information on what sciatica is, common causes, diagnosis, treatments, research, and finding medical experts.
- WebMD: Presents an overview of sciatica, including causes, symptoms, pain relief exercises, and safety considerations.
- Diagnosis and Medical Management:
- Mayo Clinic: Explains how sciatica is diagnosed, when imaging may be used, and which medical or self-care treatments may be recommended.
- NICE Guideline on Low Back Pain and Sciatica: Provides clinical recommendations for assessment, self-management, exercise, imaging, medication, and surgical referral considerations.
- Exercise and Rehabilitation Research:
- Cochrane Review on Exercise for Chronic Low Back Pain: Reviews evidence on exercise therapy for chronic low back pain and its effects on pain and function.
- Neural Mobilization for Lumbar Radiculopathy: Reviews randomized controlled trials on neural mobilization for lumbar radiculopathy and its effects on pain and disability.




